How serious is postmenopausal bleeding? Menopause is a regular event in the life of any mature woman. As you will approach menopause, your period will become lighter, shorter in duration, and it will start getting more frequent (21-26 days apart) or farther than the usual 28 days cycle.
However, if you haven’t menstruated in the last 12 months, it qualifies as menopause, and it symbolizes an end to your fertility.
Still, if you begin to spot red after you have attained menopause, it could be a red flag for more serious health concerns. In most instances, the spotting is harmless, and it could be a result of estrogen overdose, a consequence of the Hormone Replacement Therapy (HRT).
However, there lurks likelihood that the postmenopausal bleeding could be a warning sign of gynecological cancers. Therefore, if you spot post-menopause bleeding, do go visit your gynecologists to evaluate the reasons in detail.
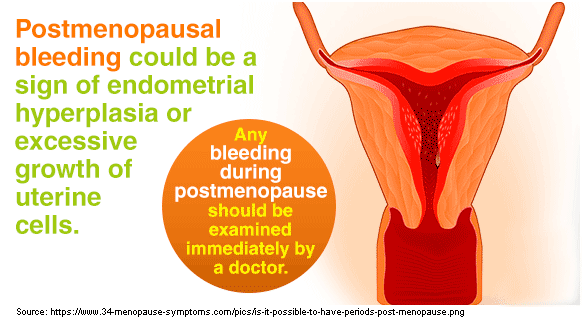
Causes of bleeding after menopause
It’s common knowledge that estrogen (the primary sex hormone) level will dip after your period stops, and you will experience uncomfortable symptoms like hot flashes and vaginal dryness. The atrophy in your vagina is the most common cause of spotting. To offset the dryness inside your vagina, your gynecologists may prescribe HRT to replace the missing estrogen hormone.
1. Hormone Replacement Therapy
The downside of estrogen replacement is postmenopausal bleeding. The uterine lining is very sensitive to estrogen, and its presence will promote the growth of uterine lining (endometrium), the way it used to during a regular menstrual cycle.
However, if you do not take synthetic estrogen, the blood vessels of your uterine lining could atrophy in its absence. They might become fragile and bleed. So, it’s a catch 22 situation.
2. Endometrial Hyperplasia
Another side effect of HRT is endometrial hyperplasia or overgrowth of endometrial lining. Estrogen acts as a growth hormone, and progesterone counters its effect, which means it helps shed the uterine lining. When estrogen becomes the dominant hormone, and there is little of progesterone to counterbalance its effect, it will cause the lining of the uterus to thicken and is a potential cause of postmenopausal bleeding. There is always a risk that endometrial hyperplasia can develop into endometrial (uterine lining) cancer if it is not treated in time.
3. Uterine polyps
Uterine polyps are soft red outgrowths on the lining of the womb. They are usually non-cancerous, but they can cause irregular bleeding post-menopause.
4. Endometrial cancer (uterine cancer)
Endometrial cancer is the most common type of uterine cancer, again because of an elevated estrogen level. About 10 percent women who experience postmenopausal bleeding have endometrial cancer. If you are above 60 and have started to bleed abnormally, it could be a warning sign of endometrial cancer. Here, a hysterectomy (removal of the uterus) is the best option in such cases.
5. Ovarian cancer
If your mother or your aunt suffered from ovarian cancer, you too, have a higher risk of getting ovarian cancer. The risk significantly increases in postmenopausal women who are on HRT and take estrogen without progesterone for a minimum of 5 to 10 years. Along with postmenopausal bleeding, you may feel bloated and experience pain in your lower abdomen.
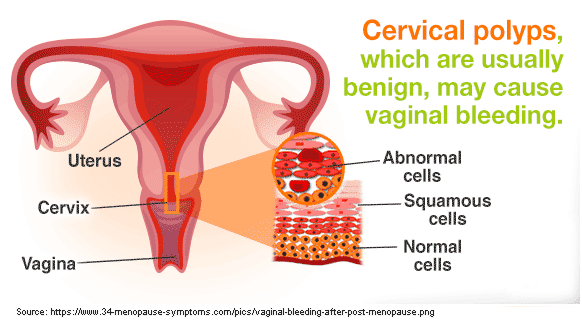
6. Cervical cancer
Cervical cancer is a cancer in the lining of the uterus. Irregular bleeding after you’ve attained menopause could be a warning sign of it. Cervical cancer is a slow-progressing disease, and regular Pap Smears can help detect any abnormal change in the cervix before it becomes malignant.
Other symptoms of Menopause
If you are like most women, you are going to experience other symptoms along with postmenopausal bleeding. The other symptoms are:
- Dryness in vagina
- Reduced libido
- Insomnia
- Stress Incontinence
- Increased urinary tract infections
- Weight gain
Diagnosis
To understand postmenopausal bleeding in detail, your doctor may ask you questions to understand your health history. She will probe to understand the timing and flow of your bleeding: when and how much?
She will most likely physically examine the insides of your vagina and may take sample tissue of your cervix to study it in detail. She may run a blood test to understand your hormonal profile in detail. Possibly, she would get an ultrasound of your pelvis done to get a picture of your internal organs: cervix, uterus, endometrium, and ovaries.
Treatment
Your treatment will largely depend on what is causing postmenopausal bleeding – from the diagnosis in the previous step.
For atrophic vaginitis, your doctor will prescribe estrogen hormone in the form of a tablet, gel, cream, skin patch or a soft, flexible ring, which is put inside your vagina and slowly releases the medication. The Progestin therapy will help if you have been suffering from the thickening of the endometrium.
If your doctor suspects the cause of bleeding as a benign growth in the ovary or cervix, which might turn cancerous in the future, she will remove the uterus.
In most cases, this bleeding is caused by stress and hormonal imbalance, and will resolve itself with time. However, the standard rule for postmenopausal bleeding is to get it examined by a gynecologist right away. By doing this, you will allow her to reckon the difference between a spotting or heavy bleeding, and she can treat it accordingly.
Related Videos:
Post Menopausal Bleeding (AUB)
https://www.youtube.com/watch?v=Y0fOm8-TyLE?autoplay=1&rel=0
Postmenopausal Uterine Bleeding
https://www.youtube.com/watch?v=HqfQkZbl0_M?autoplay=1&rel=0
Menopause & You: Bleeding After Menopause
https://www.youtube.com/watch?v=tw24nGCBFSA?autoplay=1&rel=0
Postmenopausal Bleeding
https://www.youtube.com/watch?v=0t4bVsVprOM?autoplay=1&rel=0
Postmenopausal Bleeding
https://www.youtube.com/watch?v=1jhVE-q2J4M?autoplay=1&rel=0
How serious is postmenopausal bleeding?
postmenopausal bleeding symptoms, what is the most common cause of postmenopausal bleeding?, bleeding after menopause and back pain, bleeding after 10 years of menopause, bleeding after menopause bright red, postmenopausal bleeding definition, postmenopausal bleeding ppt, light spotting after menopause causes,